What are zoonotic diseases?
COronaVIrus Disease 2019 (COVID-19) is called a zoonotic disease because the virus that causes it – Severe Acute Respiratory Syndrome COronaVirus 2 (SARS-CoV-2) – originally infected animals such as bats or pangolins. The virus jumped from one of these species to humans, although the exact animal host (the animal “reservoir”) is not yet identified.
An infectious disease that jumps from other animals to humans is called a ‘zoonotic disease’ or a ‘zoonosis’. The disease is not caused by the animal; it is usually caused by a pathogen such as a virus or a bacterium. The animal is simply a “vector”: a player in the relay race, passing on the baton of the disease to humans.
Probably the most familiar example of this is Rabies. When dogs in our locality behave aggressively and appear out of control, one big concern we have is that they could be ‘rabid’. Being bitten by a rabid dog passes on the Rabies virus (Lyssavirus) to humans, leading to infection by that virus.
Pathogens usually affect specific host(s), but sometimes they jump into a new species of hosts. This could happen because the pathogen comes across a new host that it can infect. A new zoonotic disease arises when a pathogen jumps from its normal host to humans. It could also be because new mutations allowed the pathogen (often a virus) to change or expand its previous host range, so it can now infect additional species of animals, including humans. According to some estimates, of all the new infectious diseases that we have seen in the last 30 years, over 60% are zoonotic. COVID-19 is the latest.
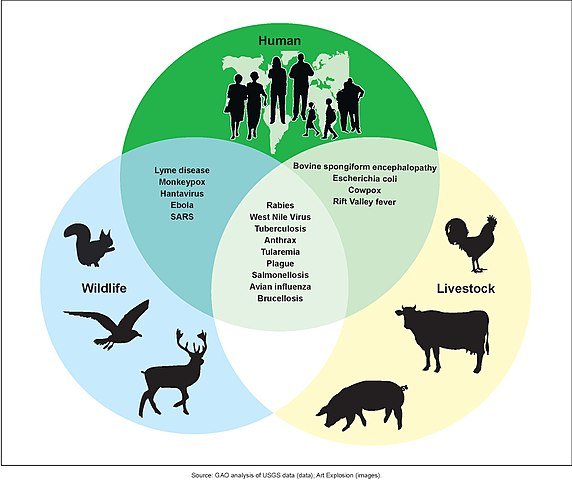
Resources
- [General] WHO: Zoonoses definition
- [General] PBS: Why Do Other Animals Keep Giving Us Viruses?
- [General] CDC: Zoonotic Diseases
- [General/HS] Facts about zoonotic diseases: What are zoonotic diseases?
- [General/HS] Overview of zoonoses, precautions to take with pets and other animals: Zoonosis: What Is All the Fuss About?
- [UG+] Descriptions of diverse zoonotic diseases: Zoonoses
Are some animals more likely to produce zoonoses? The case of bats, observation, reasons and what action would be best.
Zoonotic diseases have drawn worldwide attention in the last 20 years: with outbreaks of SARS (Severe acute respiratory syndrome, two independent outbreaks now), MERS (Middle East respiratory syndrome), Ebola, Nipah and Hendra viruses. In all of these cases, the best guess for the animal reservoir or vector turns out to be bats. This has led to the idea that bats harbour more zoonotic viruses (capable of infecting humans) than other animal species. However, careful analysis shows that the increased rate of bat zoonoses occurs because there are simply many more species of bats than most other groups of mammals. In addition, bats are widespread, they live in several different habitats, and live in and near human habitation. This increases the chance of human-bat contact. And, given that humans are more likely to be affected by viruses from other mammals (because of biological similarities), it makes sense that the most diverse (i.e. species-rich) mammals could serve as the original hosts of most viruses that jump to humans. Similarly, rodents are another class of mammals that are ‘species rich’, and have also contributed to zoonoses in the past.
It is important to remember that in several cases, once a closely related virus was identified in a bat (Ebola, SARS, SARS-CoV-2), scientists stopped screening other potential animal hosts. This makes it hard to determine the precise source of the virus that made the jump to humans. Our estimate of the number of zoonoses is also limited to infections that not only make the initial jump from an animal to a human, but then also successfully move from one human to another. If the chain of transmission does not extend to other humans, a zoonosis may only cause small, local outbreaks instead of escalating to an epidemic or pandemic level.
Resources
- [HS/UG] Zoonotic diseases: Why are infections from animals so dangerous to humans? Suggests a combination of causes — our immune system, natural selection and the specific animal that transmits the virus; discusses what might have happened in COVID-19
- [UG+] Coronavirus outbreak raises question: Why are bat viruses so deadly? Bats’ immune system might allow them to carry high numbers of viruses (virus load) without falling sick.
How often do zoonotic events occur? Have they increased recently? Why?
From 1980 to 2013, the global incidence of zoonotic disease outbreaks has increased, even after controlling for many confounding factors such as geography and surveillance structure. There are now over 3 times as many zoonotic outbreaks as in the 1980s, and they are caused by a more diverse set of pathogens.
Viruses (the most common source of recent zoonotic diseases) mutate rapidly, continually producing new viruses in animal hosts. Most of these mutants get weeded out because they have lower survival. Some, however, are improved versions and may either cause more severe disease or acquire the ability to jump to a new host. Although in itself a rare event, the large number of such viruses combined with increasing human-animal contact is thought to cause the increase in zoonotic infections.
Studies show that human activities greatly influence the spread of zoonotic diseases. For example, habitat destruction such as large scale deforestation and forest fragmentation can lead to the migration of wildlife into human habitats. Cutting down huge stretches of forest within a short span of time leaves several wild animals and birds homeless, causing them to move away from these wild areas. In our crowded world, migration to areas outside of a forest nearly always leads to greater contact with human societies. Like habitat destruction, increased forest fragmentation and climate change (leading to habitat change) also displaces local wildlife and increases human-animal contact. In addition to increasing dangerous physical human-animal conflicts, this can also trigger zoonotic events.
Other factors also play a role. For example, illegal trafficking and hunting of exotic animals and animal products brings people into contact with animals that they would otherwise encounter only rarely. Consuming live animals, especially wild species (bushmeat), does the same. Even people that are not directly engaged in hunting or trafficking can be exposed to pathogens from wild animals at large markets where such animals or their parts are sold. Similarly, large-scale animal husbandry also places people in close contact with many animals. It is thus not surprising that humans share the largest number of viruses with domesticated mammals.
Resources
- [General] How do viruses mutate and jump species? And why are ‘spillovers’ becoming more common?
- [General] Deforestation and disease: How natural habitat destruction can fuel zoonotic diseases
- [General] Research Suggests Climate Change Could Favor Zoonotic Diseases
What can we do to limit the emergence of new zoonotic diseases?
Human activities increasingly encroach on forest cover and destroy existing habitats, increasing the chances of close contact with various species of wildlife. The current CoViD-19 pandemic (and others in recent years) adds a significant human cost to environmental damage.
A critical aspect is to reduce the risk of pathogen transmission to people who work with wild and domestic animals; e.g. by improving biosafety measures. It is important to do/ conduct regular surveillance of pathogens in domestic and wild animals as well as in the people who come in contact with them to reduce the spread of zoonotic diseases. In addition, to reduce the emergence of zoonoses, experts have advocated for strong global measures to abolish illegal trade in wildlife, minimize encroachment in wildlife refuges, and mitigate the loss and fragmentation of natural habitats. In our hyper-connected world, minimizing pandemics is a serious and complex problem that requires not only global response measures, but also regional frameworks that are finely tuned to specific local contexts.
Resources
- [UG+] Ecology of zoonoses: natural and unnatural histories: An overview of the ecology of zoonoses showing the need for using ecological and evolutionary understanding of diverse factors in an evidence-based decision making to help reduce zoonoses.